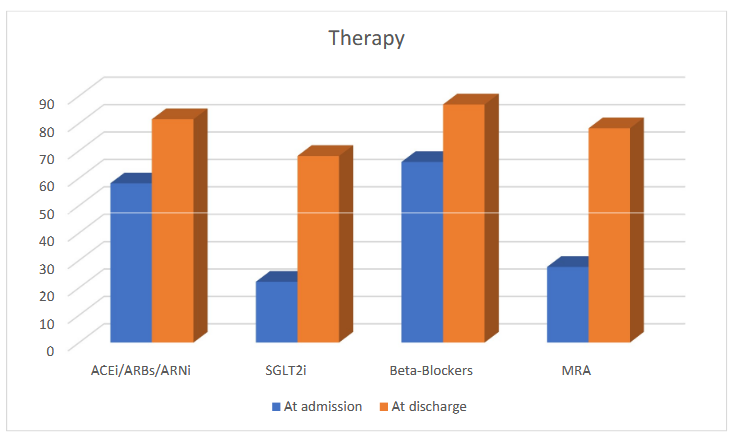
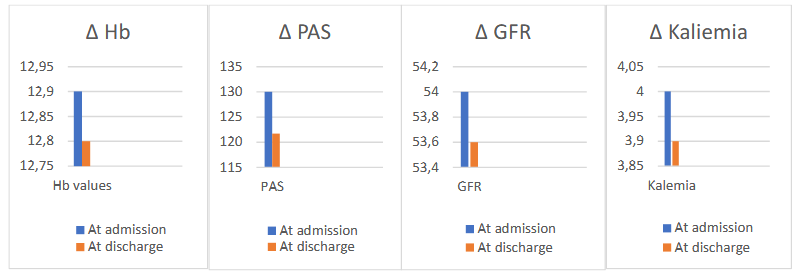
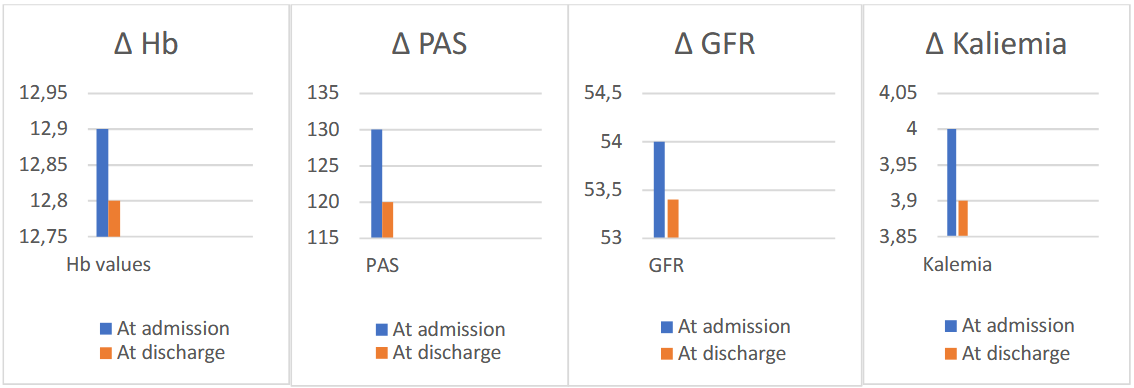
Introduction Growing evidence supports early and intensified therapy during hospitalization for acute decompensated heart failure (ADHF) to reduce cardiovascular morbidity and mortality across the entire spectrum of ejection fraction (EF). Trials such as EMPULSE and TRANSITION have demonstrated that early initiation of empagliflozin and sacubitril/valsartan in hospitalized patients with ADHF is feasible and safe. Purpose This study aimed to evaluate the safety and tolerability of an early and accelerated implementation of guideline-directed medical therapy, with particular focus on the four therapeutic pillars, during hospitalization for ADHF. Methods We retrospectively analyzed 373 consecutive patients admitted from the Emergency Department to our Cardiology Unit between August 2023 and December 2024. Utilization of the four pillars at admission and discharge was compared, along with changes in systolic blood pressure (SBP), creatinine, estimated glomerular filtration rate (eGFR), NT-proBNP, serum potassium, and hemoglobin levels. Results Median age was 79 years, 59.5% were male, median BMI was 25.9, and 23.6% had diabetes. Heart failure phenotypes included HFrEF (27.6%), HFmrEF (26.8%), and HFpEF (45.6%). Use of ACEi/ARBs/ARNi increased from 58.1% at admission to 81.5% at discharge. SGLT2 inhibitor prescription rose from 22.2% to 68.1%. Beta-blocker use increased from 65.9% to 86.9%, and MRA use from 27.6% to 78.2%. During hospitalization, hemoglobin decreased slightly (12.9 ± 1.9 to 12.8 ± 2.0 g/dL; p=0.03) and SBP declined from 130 (115–145) to 120 (110–130) mmHg (p<0.0001). Renal function showed a modest but significant worsening, with creatinine increasing from 1.19 to 1.24 mg/dL (p=0.0045) and eGFR decreasing from 54 to 53.4 mL/min (p=0.0021). Serum potassium levels slightly decreased from 4 (3.7-4.3) to 3.9 (3.7-4.2) mEq/l (p=0.009) Among patients not receiving SGLT2 inhibitors,only 5.6% had an absolute contraindication (eGFR <25 mL/min). NT-proBNP levels significantly decreased from 3068 (1396-7004) to 2276 (941-5126) (p<0.0001). Discussion Hospitalization represents a crucial opportunity for therapeutic optimization in ADHF. Early initiation of intensified therapy was feasible, safe, and well tolerated, with only modest and expected changes in clinical and laboratory parameters. The low rate of absolute contraindications to SGLT2 inhibitors suggests that therapeutic inertia may significantly contribute to their underutilization.