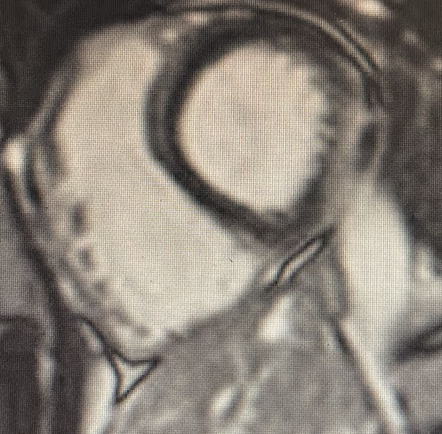
A 44-year-old man presented to the emergency department with progressive dyspnea, peripheral edema, and fever lasting several days. He had no cardiovascular risk factors and had recently returned from Thailand. Initially admitted with suspected pneumonia, he rapidly developed hypotension and anuric acute kidney injury and was transferred to the intensive care unit with mixed shock. Aggressive volume resuscitation and catecholaminergic support with adrenaline (up to 0.1 µg/kg/min) were initiated. Cardiac catheterization revealed pulmonary hypertension (CI 5,5 L/m PAPs/m/d 65/45/37 mmHg, PAWP 35 mmHg, PVC 20 mmHg, PVR 2 Wood units), leading to the initiation of sildenafil. The patient was subsequently transferred to our Cardiac Intensive Care Unit (CICU) for further evaluation. Transthoracic echocardiography showed a severely dilated and hypokinetic right ventricle with diastolic left ventricular compression and mildly reduced left ventricular systolic function (LVEF 45%) with diffuse hypokinesia. Marked systemic venous congestion was evident, including systolic flow reversal in the hepatic veins, portal vein pulsatility >30%, and purely diastolic renal venous flow. Repeat right heart catheterization demonstrated a high-output state with pulmonary hypertension and normal pulmonary vascular resistance (CI 6 L/min/m²; PAP 64/37/25 mmHg; PAWP 13 mmHg; mean right atrial pressure 21 mmHg; PVR 2 Wood units). Infectious etiologies, intra- and extracardiac shunts, and thyroid dysfunction were excluded. Thiamine supplementation was initiated due to suspicion of beriberi. Despite the absence of a definitive diagnosis, a physiology- and hemodynamics-guided strategy was adopted: adrenaline was discontinued, and aggressive decongestive therapy was implemented. After achieving a cumulative negative fluid balance greater than 10 L, normalization of venous congestion indices, pulmonary pressures, and right ventricular function was observed. Cardiac magnetic resonance imaging showed non-ischemic late gadolinium enhancement in the basal inferior and inferolateral segments, consistent with inflammatory myocardial injury. Conclusion : this case underlines the importance of a hemodynamic- and congestion-focused approach in severe cardiac dysfunction. Even in the absence of a clear etiology, targeted decongestion led to reversal of myocardial and renal dysfunction, highlighting the central role of venous congestion in acute heart failure syndromes.