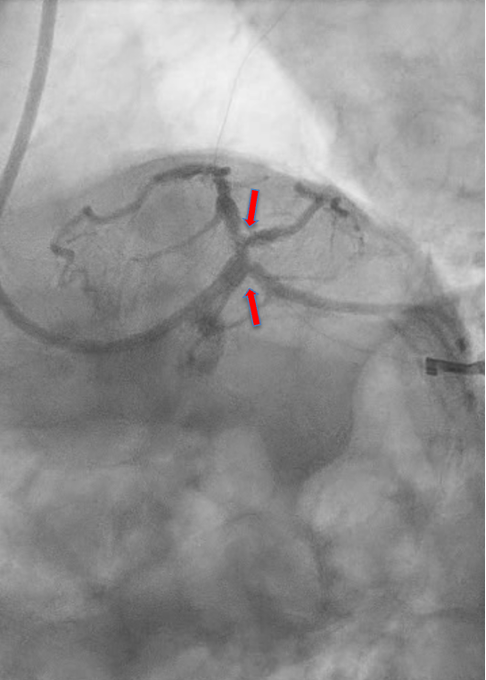
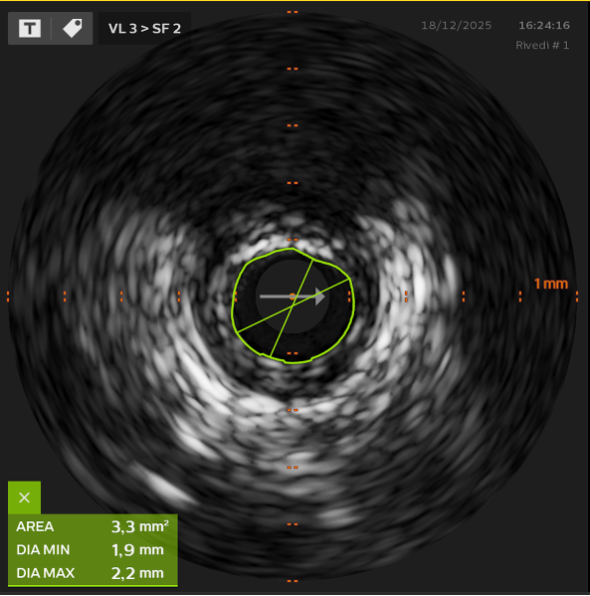
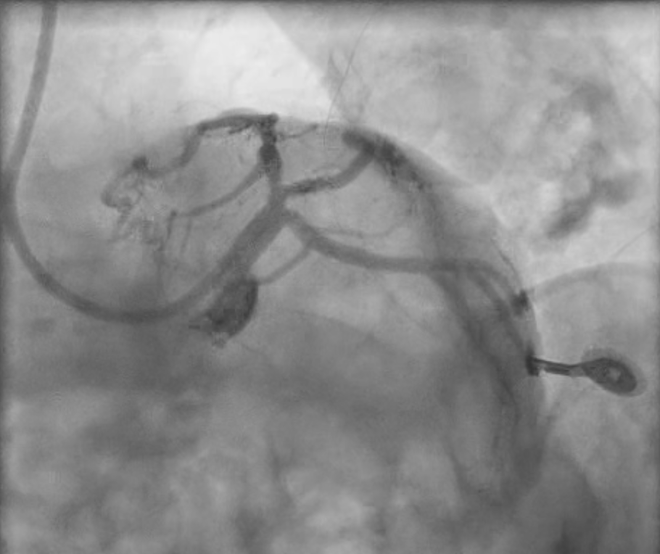
Introduction Management of multivessel coronary artery disease (MVD) in patients with recurrent acute coronary syndromes (ACS) remains challenging, particularly in the presence of several cardiovascular (CV) risk factors and previous percutaneous coronary interventions (PCI). Coronary bifurcation lesions further increase procedural complexity and are associated with higher risk of adverse events related to multiple stent implantation. Case Presentation A 50-year-old man with several CV risk factors was admitted to our catheterization laboratory for chest pain with a diagnosis of inferior ST-elevation myocardial infarction (STEMI). In 2019 the patient had a non-STEMI treated with PCI and drug-eluting stent (DES) implantation of the diagonal branch; in 2024 he underwent to a PCI with DES implantation of the proximal left anterior descending artery (LAD) for an anterior STEMI. Coronary angiography revealed an acute thrombotic occlusion of the posterior interventricular branch (PDA), significant stenosis of the ostial left circumflex artery (LCx), and in-stent restenosis of the LAD and of the diagonal branch (D1). Primary PCI with DES implantation of the PDA was successfully performed; after the procedure the patient was transferred in the Coronary Care Unit. After five days the patient underwent to PCI staged procedure to achieve complete revascularization. Intravascular ultrasound (IVUS) assessment of the LAD and LCx revealed significant in-stent atherosclerosis of the LAD and a concentric fibro-lipidic plaque with small amount of calcium at the ostium of LCx, with a Minimal Lumen Area (MLA) of 3.3 mm 2 . Pre-dilatation with a kissing balloon (KB) technique using two non-compliant (NC) balloons 3.0×15 mm inflated at high atmospheres, was performed on the LAD and LCx, followed by NC balloon dilatation 2.5×20 mm of the D1. In order to avoid additional stent implantation, we decided to perform a final KB on the LAD and LCx with two Sirolimus drug-eluting balloons (DEB), obtaining an optimal angiographical result. Follow-Up At 6-months follow-up, the IVUS demonstrated absence of neo-atherosclerosis of the LAD and an optimal MLA of the ostial LCx, with no evidence of adverse vessel remodelling. Conclusions This case supports the feasibility and safety of an IVUS-guided DEB strategy in complex bifurcation lesions, enabling effective revascularization while minimizing further stent implantation in a high-risk patient with MVD and recurrent ACS.