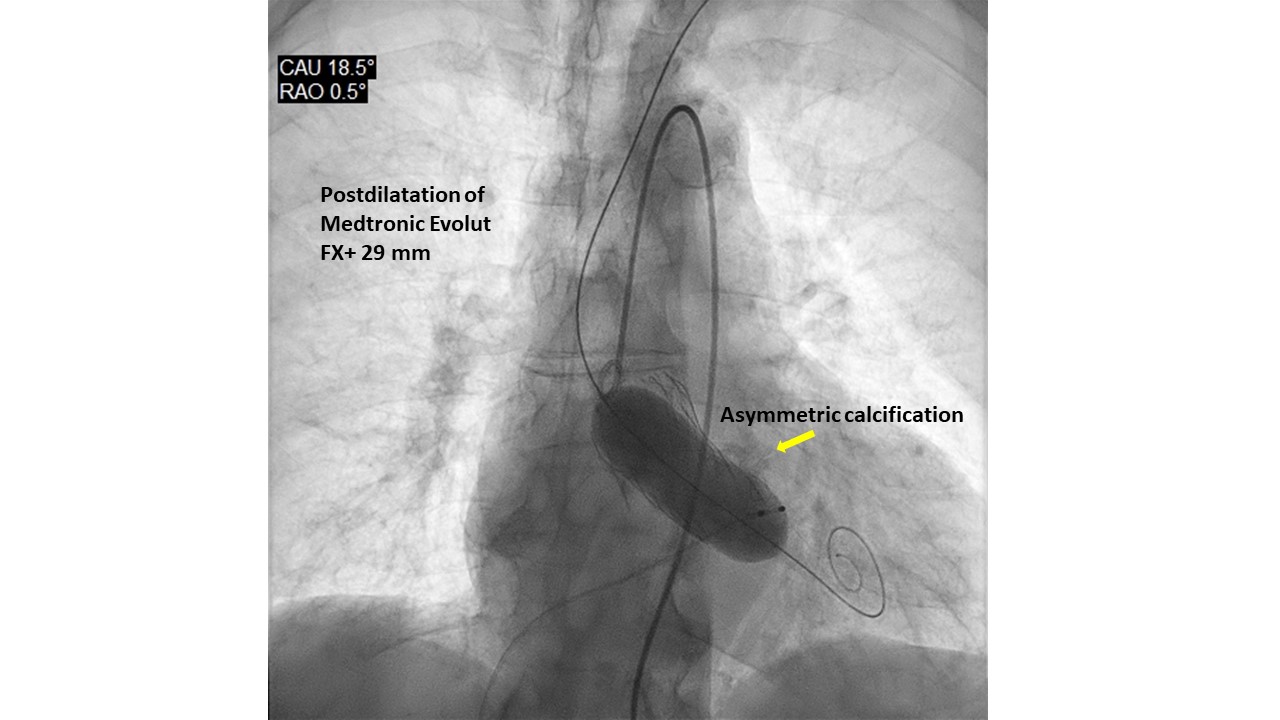
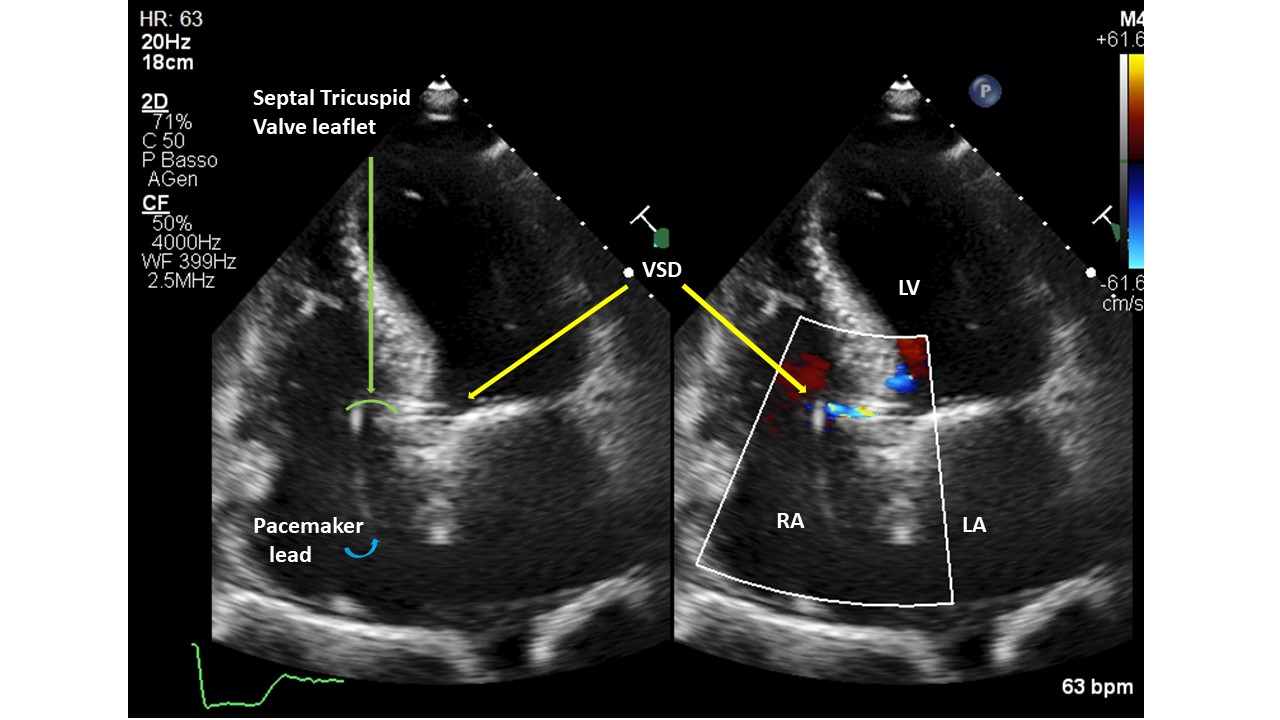
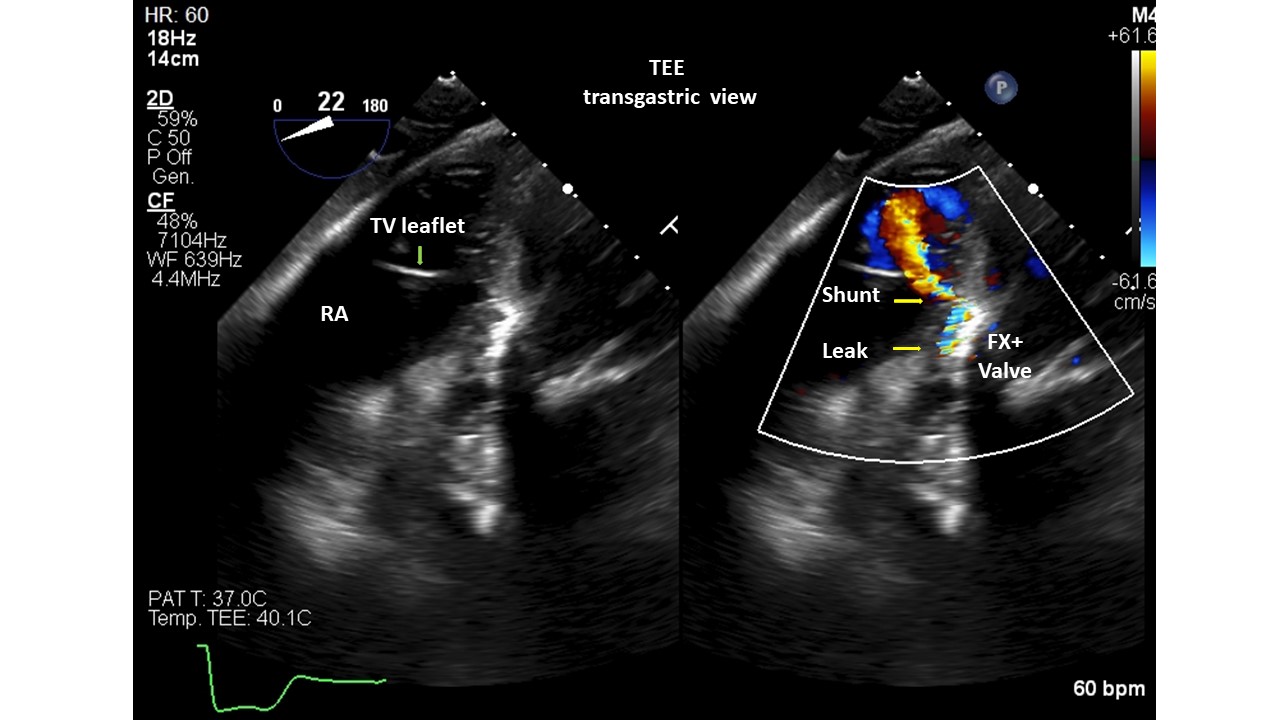
Introduction. Gerbode’s defect dates back to 1857. It generally has a congenital etiology, however very rare acquired forms have been described as complications of cardiac surgery, bacterial endocarditis, thoracic trauma, myocardial infarction or Transcatheter Aortic Valve Implant (TAVI). Diagnosing the communication between the left ventricle and the right atrium post-TAVI is not always easy, but a thorough echocardiography can lead to the correct diagnosis. We present 2 patients with Gerbode's defects post-TAVI, presumed with post-procedural transthoracic echocardiography (TTE) and validated with transesophageal (TEE) or 3D-ultrasound (3DTTE). Methods. A single-centre retrospective study of 1309 consecutive with severe aortic stenosis patients, who underwent TAVI from 2020 to 2025, was conducted with 5 types of aortic valve. All patients were evaluated with TTE before and after the procedure; only 23 patients underwent TEE. Results. Screened patients had a mean age of 82±7 years. Patients had multiple cardiac and non-cardiac comorbidities and high logistic EuroSCOREs and STS scores. Two subjects (0.15%) were found to have a Gerbode-type II septal defect. They were implanted with Medtronic Evolut FX+ valve. The calcium score of the aortic valve annulus was calculated in the 2 patients with CT (3,296 and 2,395 AU, respectively). Both prostheses were postdilated with a balloon to treat residual moderate paravalvular regurgitation. The cases were diagnosed with TEE/3DTTE to have a restrictive left to right shunt (Qp:Qs=1.4 case 1, 1.2 case 2). The patients were not symptomatic and did not require any further intervention. The mechanisms proposed for ventricular septal defect (VSD) formation: pressure exerted directly by the valve on the membranous septum, severe/asymmetric calcification of native valve, aggressive postdilatation. Conclusions. The role of TEE/3DTTE in the accurate diagnosis of these VSD suggests that it can be used as an alternative to other diagnostic tools, such as cardiac catheterization, CT and cardiac magnetic resonance imaging. Gerbode’s defect is a rare complication of TAVI and was detected more with balloon expandable valves, but can also occur with self-expanding ones. Percutaneous treatment was preferred over open cardiac surgery. Some, but not all, patients survived TAVI and VSD, and had a good prognosis for both patient groups with or without VSD closure. Careful follow-up with a dedicated team is essential in these patients.