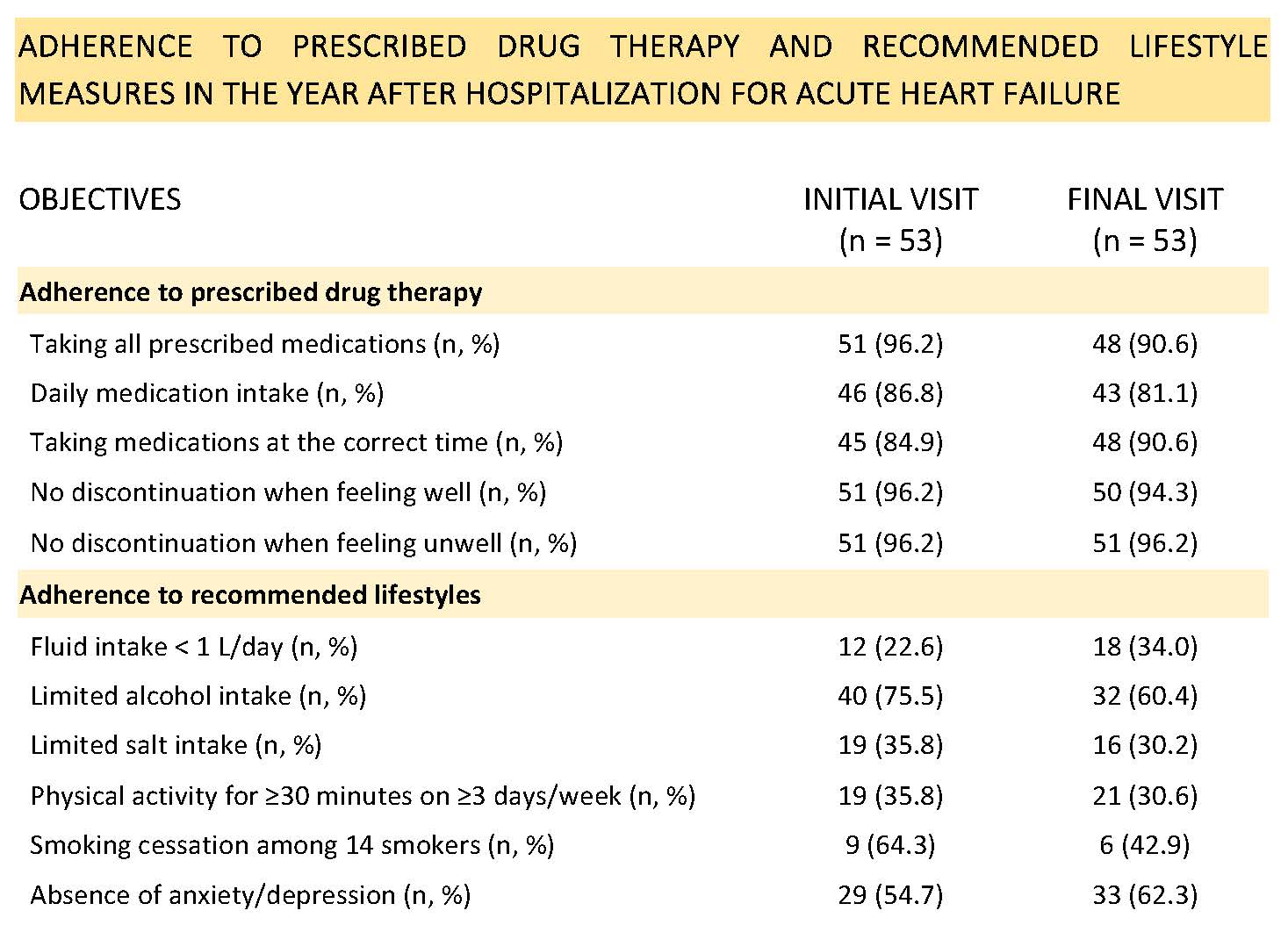
Background The first year after admission for Acute Heart Failure (AHF) is the most critical period, with high mortality and readmission rates, often favoured by discontinuation of prescribed therapies or poor adherence to lifestyle recommendations. The DIM ACC Project (“ Dim issioni Acc ompagnate”, i.e. Accompanied Discharge) was launched on May 1st, 2023 to provide a structured follow-up for patients admitted with AHF to the Intensive Cardiac Care Unit (ICCU) and Cardiology ward of Pio XI Hospital in Desio. Aim To assess adherence to pharmacological therapies and lifestyle recommendations during the first year after discharge. Methods DIM ACC is a prospective quality improvement study conducted in real-world clinical practice. Follow-up includes a structured pathway of physician–nurse visits and diagnostic tests over 12 months. Adherence to pharmacological and non-pharmacological therapies was collected by nurses during follow-up visits. Comparisons between initial and final visits were performed using the chi-square test, considering a p-value < 0.05 as statistically significant. Results From May 1, 2023, to April 30, 2024, 158 patients were admitted for AHF to our ICCU and Cardiology ward. Of these, 136 were discharged home or to a cardiovascular rehabilitation centre, and 68 were included in the project. Among these patients, 7 did not attend the first follow-up visit, 2 died before the final visit, 8 were lost to follow-up, and 53 completed the 12-month follow-up. The percentage of the latter patients reporting good adherence to pharmacological therapies and recommended lifestyle measures at the initial and final visits is shown in Table 1. At the beginning of follow-up, adherence to pharmacological therapies prescribed at discharge was very high, in contrast to adherence to recommended lifestyle measures. No statistically significant changes were observed during follow-up for any of the variables considered. Conclusion A structured follow-up after AHF hospitalization supports long-term adherence to pharmacological therapies, but has limited impact on lifestyle modification. New strategies are needed to improve patients’ diet, physical activity, smoking cessation, and psychological well-being.