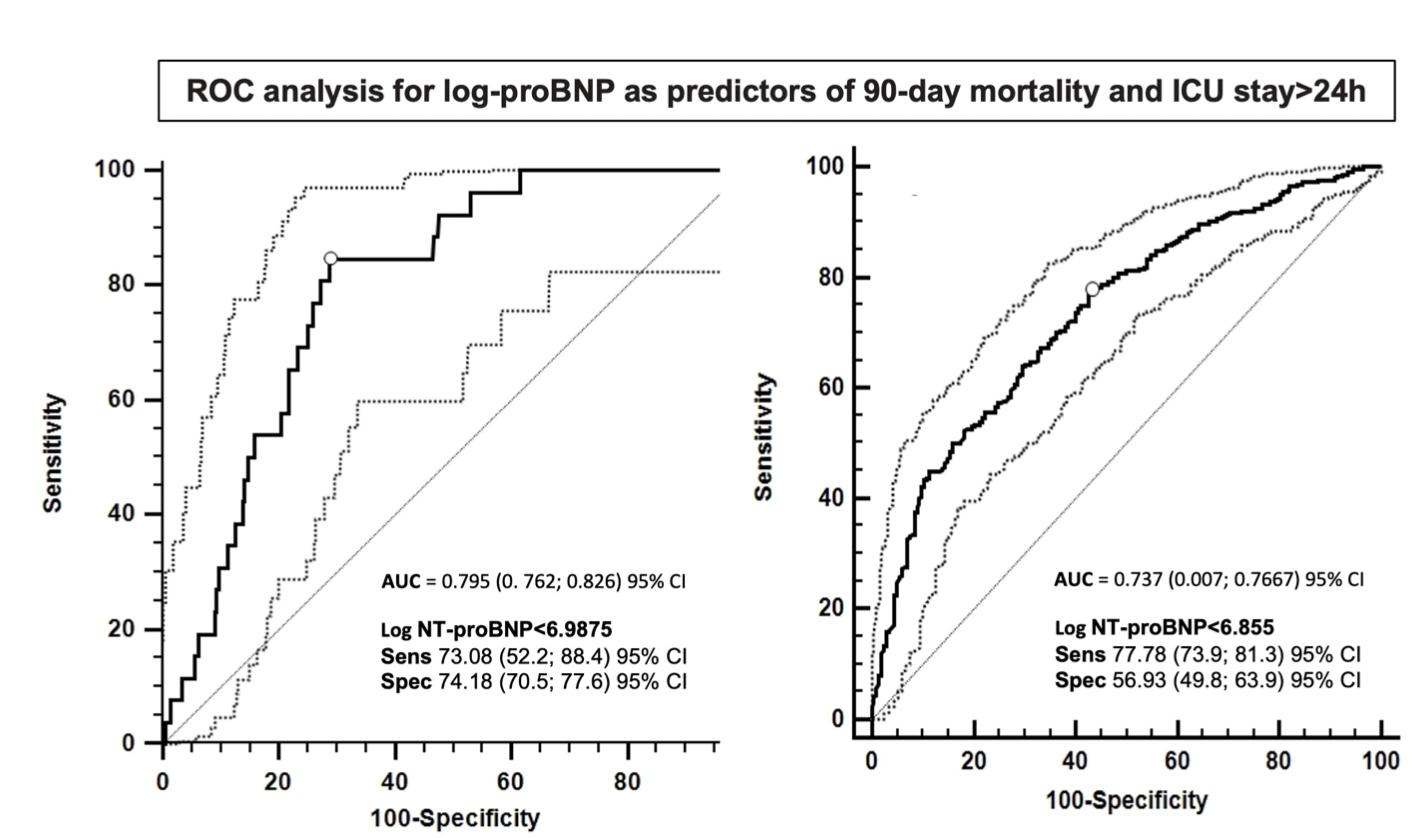
Background NT-proBNP is widely recognized as a prognostic marker in congestive heart failure. However evidence regarding its role in patients with valvular heart disease, particularly in those undergoing cardiac surgery, remains limited. Objective To analyze the association between NT-proBNP levels and mortality and peri-operative outcome in patients undergoing mitral valve surgery. Methods NT-proBNP levels were measured before, at five days, at three months and during follow-up after surgery in patients from 2020 to 2025. Primary endpoint was the prognostic value of NT-proBNP on 90-day mortality. Secondary outcomes included major post-operative complications and length of stay. Associations were assessed using univariate and stepwise multivariate logistic regression analysis. Due to their skewed distribution, NT-proBNP values were logarithmically transformed. Values that best discriminated patients outcome were identified by evaluating the ROC curves: the selected cutoff was the one that maximized sensitivity and specificity (Youden index). The statistical significance level was set at p<0.05. Statistical analysis was performed using SAS® 9.4 software (SAS Institute Inc, Cary N.C. USA). Results 797 patients were enrolled, with a mean age of 67 years; 361 patients (45.3%) were female and 137 (17.2%) had previous cardiac surgery. In-hospital and 90-day mortality rates were 1.6% e 3.5%, respectively. Stroke rate was 1.3%, acute kidney injury was 7% and LCOS 1.8%. Median ICU and in-hospital length of stay were 1 and 7 days, respectively. At univariate analysis, NT-proBNP was significantly associated with 90-day mortality (OR 1.906, 95% CI 1.456-2.495), ICU stay > 24 hours (OR 1.821, 95% CI 1.602- 2.071) and LCOS (OR 1.620, 95% CI 1.149-2.283). ROC curve analysis identified a logNTproBNP level of 6.99 as the threshold with the best discriminative ability for 90-day mortality, and a level of 6.86 for an ICU length of stay > 24 hours. In the multivariable model, independent predictors of 90-day mortality included NT-proBNP levels (OR 1.674, 95% CI 1.230-2.277), age (OR 1.080, 95% CI 1.020-1.143) and cardiopulmonary bypass time (OR 1.016, 95% CI 1.008-1.025). After adjustment for the selected covariates, NT-proBNP remained significant. Conclusions NT-proBNP is an important independent predictor for peri-operative outcomes and early mortality in patients undergoing mitral valve surgery, supporting its potential role in pre-operative risk stratification.