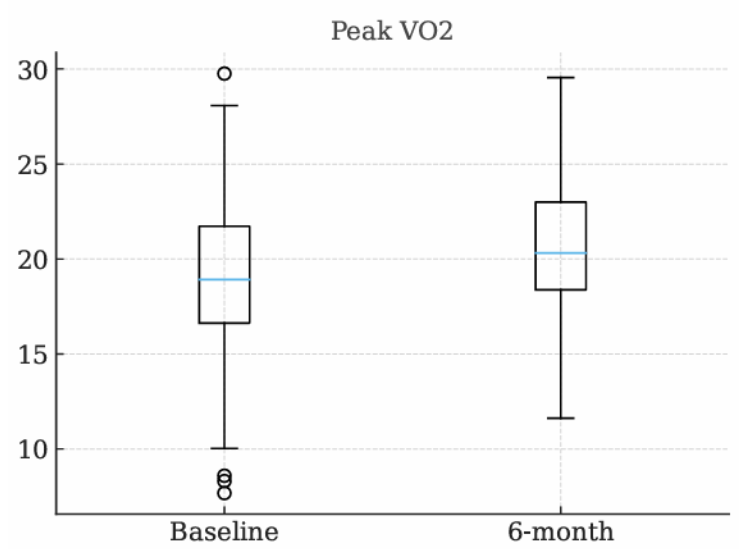
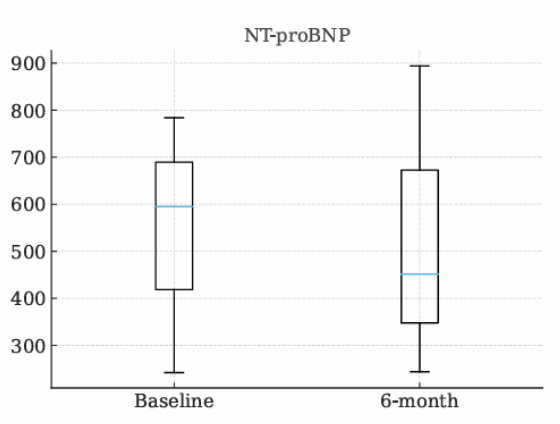
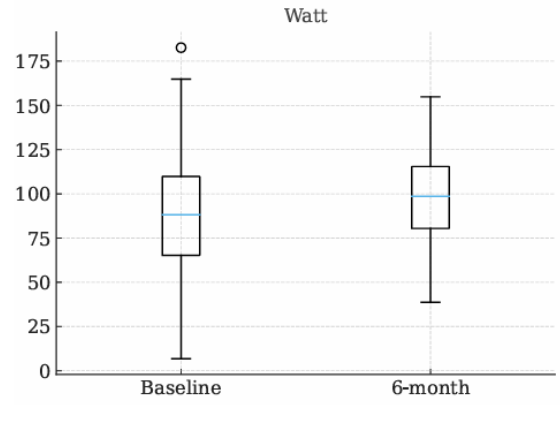
Background: Patients with nonobstructive hypertrophic cardiomyopathy (nHCM) frequently present with exertional intolerance and features of heart failure with preserved ejection fraction (HFpEF). Although sodium–glucose cotransporter 2 inhibitors (SGLT2i) have shown clinical benefit in HFpEF, patients with hypertrophic cardiomyopathy have been excluded from major randomized trials, leaving a relevant unmet therapeutic need. Methods: This longitudinal, observational multicenter study evaluated the effects of SGLT2 inhibitors on functional capacity and quality of life in patients with nHCM treated with empagliflozin or dapagliflozin, prescribed according to current cardiological indications for diastolic dysfunction. All patients had genetically confirmed nHCM and evidence of structural, functional, or serological abnormalities consistent with diastolic dysfunction. Baseline assessment and six-month follow-up included clinical evaluation, cardiopulmonary exercise testing (CPET), Kansas City Cardiomyopathy Questionnaire (KCCQ), and NT-proBNP measurement. This abstract reports preliminary data from the first ten patients enrolled at the coordinating center of Piacenza, within an ongoing multicenter project involving Ospedale Maggiore di Parma, Policlinico di Milano, Centro Cardiologico Monzino, Ospedale di Messina, Ospedale di Palermo, Ospedale di San Benedetto del Tronto, and Ospedale di Verona. Results: Baseline peak oxygen uptake (VO₂) was 19.1 ± 3.7 mL/kg/min, indicating mild-to-moderate functional limitation, and increased to 20.7 ± 3.8 mL/kg/min at six months (p = 0.415). Oxygen pulse rose from 12.3 ± 2.8 to 13.1 ± 2.5 mL/beat (p = 0.476), while ventilatory efficiency improved, with VE/VCO₂ slope decreasing from 30.5 ± 6.8 to 28.9 ± 5.2 (p = 0.221). Maximal workload increased from 89.7 ± 31.4 to 98.7 ± 25.4 W (p = 0.109). KCCQ-CSS showed a favorable trend (84.8 ± 11 to 86.5 ± 13; p = 0.332). NT-proBNP decreased from 595 pg/mL (IQR 242–784) to 451 pg/mL (IQR 244–894; p = 0.262). Conclusions: Although statistical significance was not achieved, likely due to the limited sample size, all analyzed parameters showed a consistent trend toward improvement. These preliminary findings suggest a biologically coherent benefit of SGLT2 inhibition in patients with nHCM and an HFpEF phenotype, supporting further investigation in larger multicenter studies.