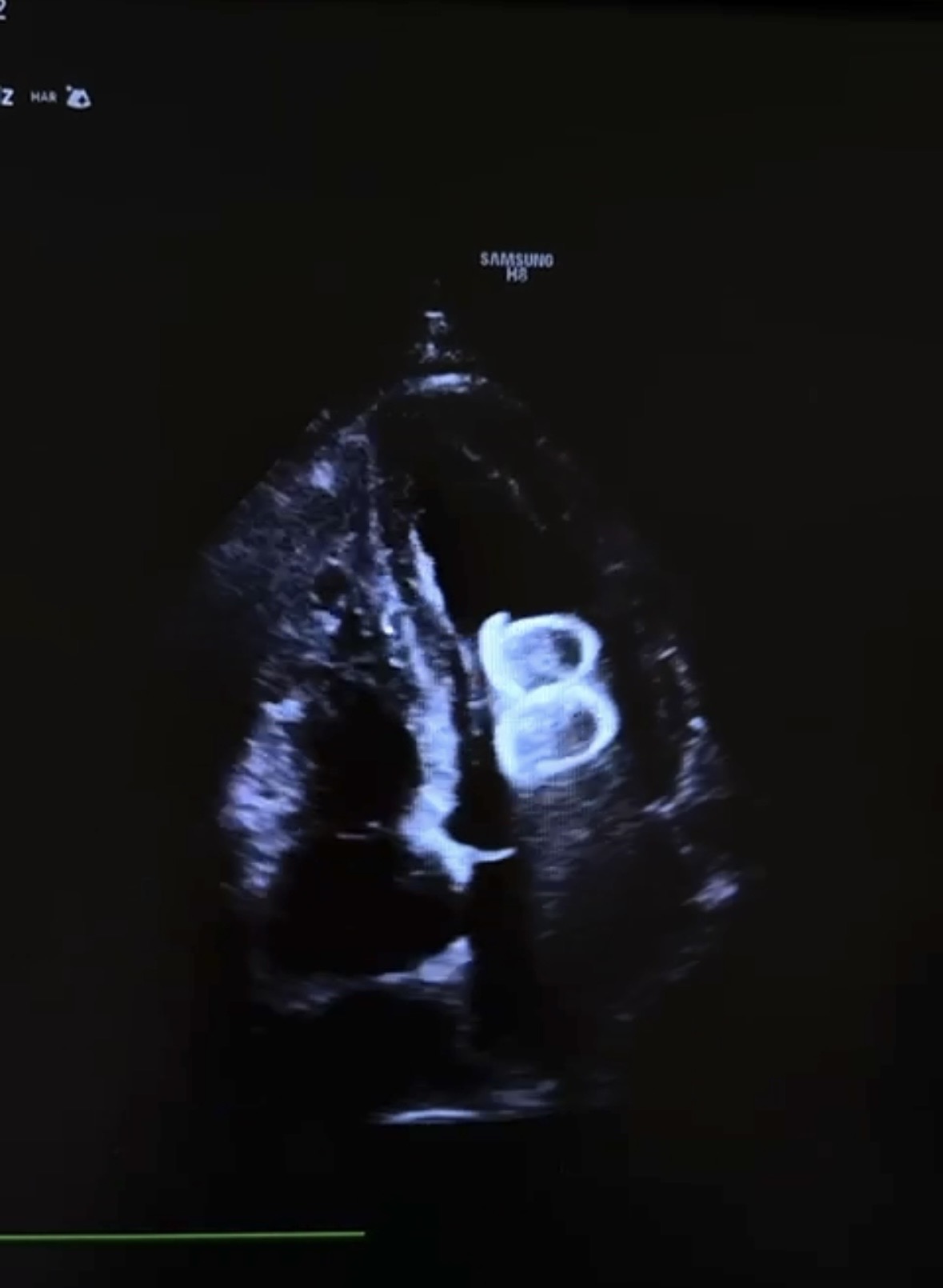
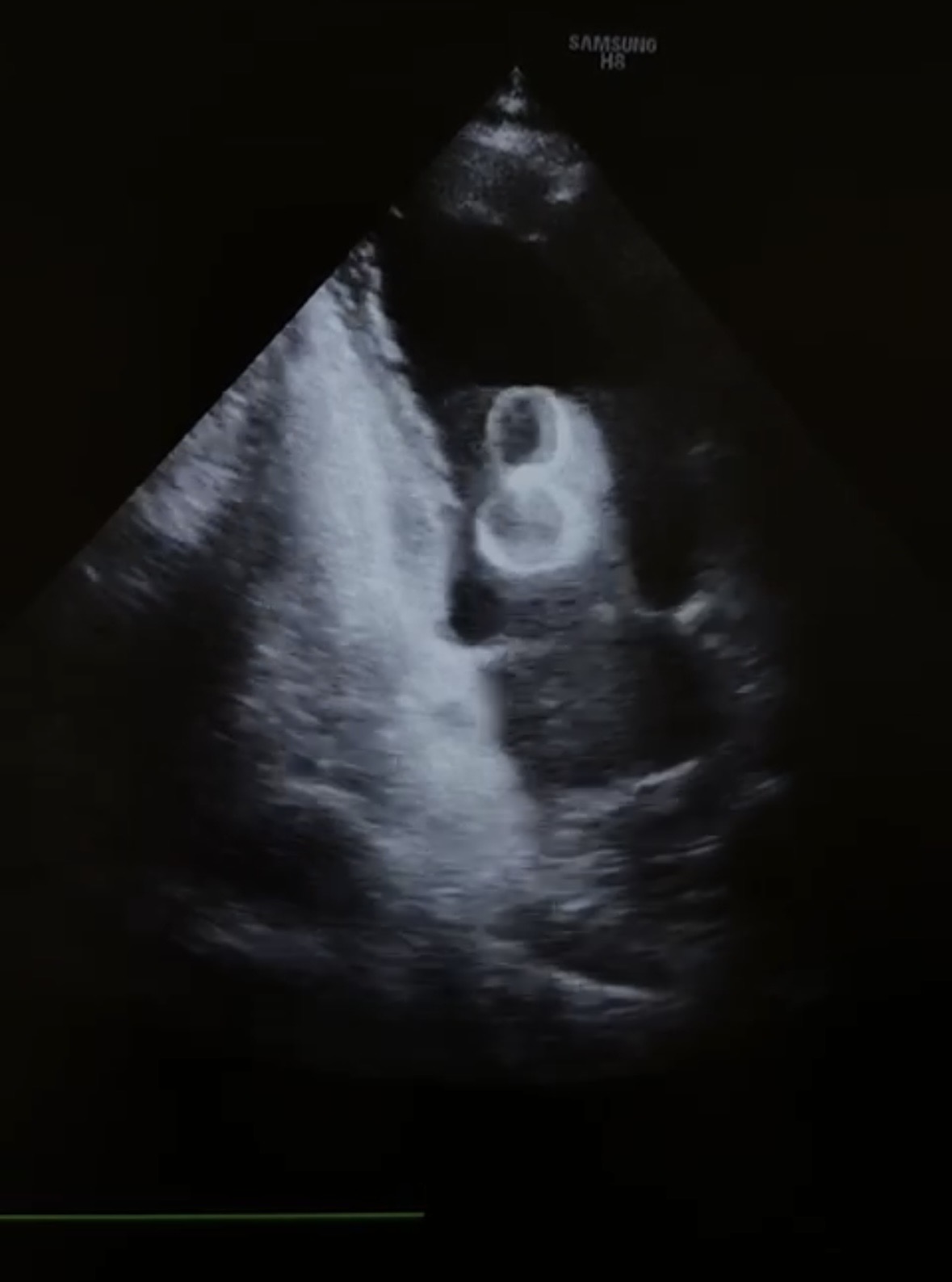
A male patient in his seventies was admitted for percutaneous left atrial appendage closure (LAAc). The indication for the procedure was paroxysmal atrial fibrillation in the setting of a previous hemorrhagic stroke that occurred during treatment with a non–vitamin K antagonist oral anticoagulant (NOAC), making long-term anticoagulation contraindicated. The procedure was performed under transesophageal echocardiography (TEE) guidance. A meticulous pre-procedural assessment of left atrial appendage anatomy was carried out, including evaluation of the ostium, depth, and landing zone. Device sizing was considered appropriate, and stability was confirmed intra-procedurally by standard tug (pull-and-release) maneuvers. Final angiographic and echocardiographic assessments suggested correct positioning and adequate sealing, and the procedure was concluded without immediate complications. Following the intervention, the patient was transferred to the intensive care unit for routine post-procedural monitoring. Shortly after admission, he developed recurrent episodes of non-sustained ventricular tachycardia. Given the abrupt onset of ventricular arrhythmias, an urgent bedside transthoracic echocardiogram was performed. This revealed the presence of a mobile, hyperechoic structure within the left ventricular cavity, highly suggestive of device embolization. Emergency cardiac surgery was immediately consulted, and the patient was transferred to the operating room without delay. Surgical exploration confirmed embolization of the LAA occlusion device into the left ventricle. The device was successfully retrieved, and definitive exclusion of the left atrial appendage was achieved surgically using a single suture. The postoperative course was uneventful, with resolution of ventricular arrhythmias and hemodynamic stabilization. This case highlights device embolization as a rare but potentially catastrophic complication of percutaneous LAA closure. Even when optimal sizing, imaging guidance, and stability testing are performed, late embolization can occur. Sudden ventricular arrhythmias in the early post-procedural period should raise immediate suspicion for device migration, and prompt echocardiographic evaluation is crucial. Rapid multidisciplinary collaboration is essential to ensure timely diagnosis and life-saving intervention.