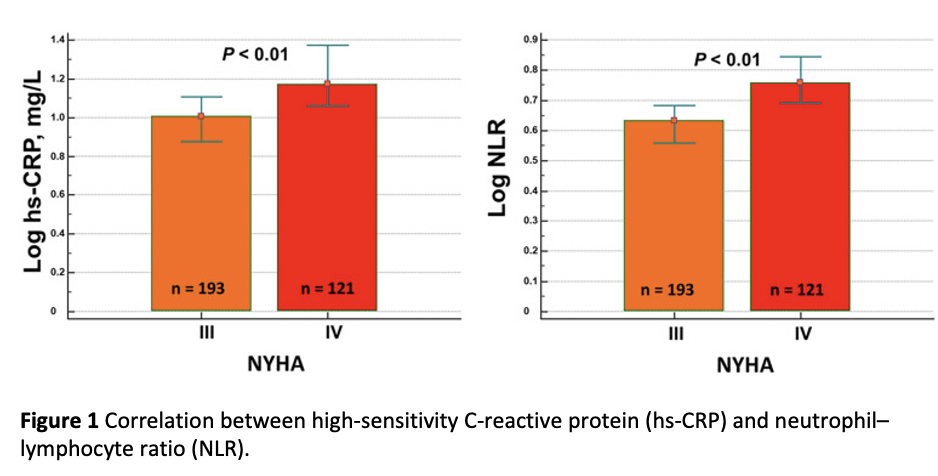
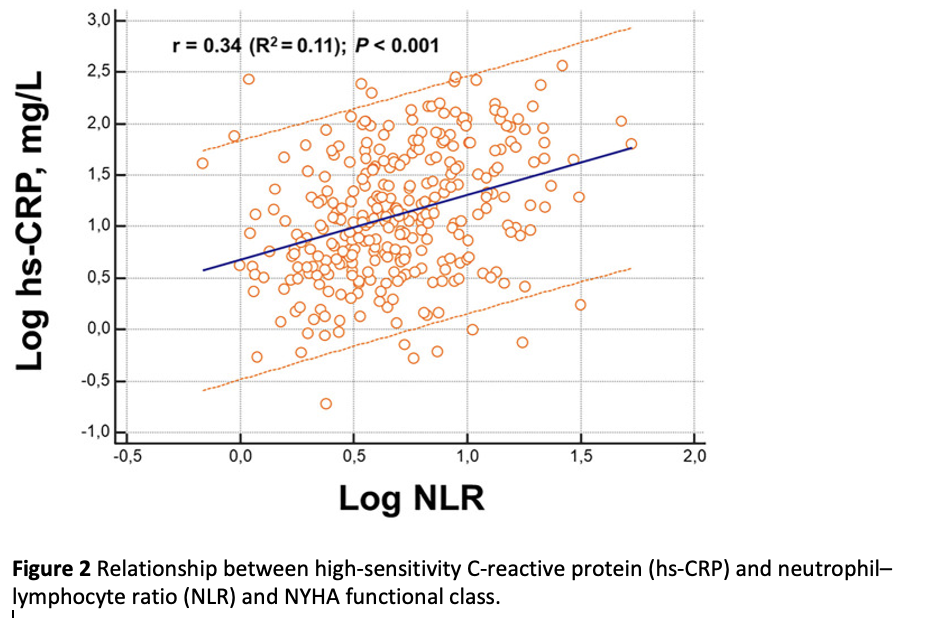
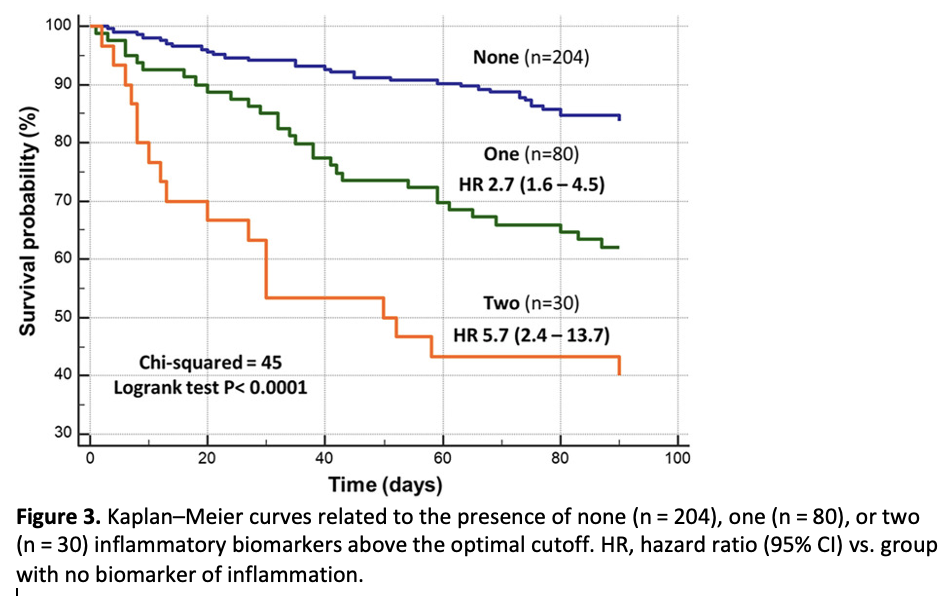
Background: The reciprocal correlation between systemic inflammation and heart failure (HF) is a hotline research topic although the exact role in risk stratification and prognosis within the acute setting is a matter of debate. This study aimed to evaluate the correlation among two inflammatory biomarkers- namely, high-sensitivity C-reactive protein (hs-CRP) and neutrophil-lymphocyte ratio (NLR), congestion status, and prognosis in patients with acute HF (AHF). Methods: We consecutively enrolled 314 AHF patients. Congestion biomarkers [brain natriuretic peptide, estimated plasma volume status (ePVS), hydration index (HI), blood urea nitrogen to creatinine ratio (BUN/Cr)] were evaluated to assess hemodynamic intravascular, peripheral, and venous congestion. We also measured hs-CRP and NLR as markers of inflammation. The endpoint was all-cause mortality at 90 days. Results: hs-CRP concentrations at admission [12.1 mg/L, 95% confidence interval (CI) 10-15] were associated with NLR values (4.8, 95% CI: 4.3-5.3) (R 2 = 0.11; p < 0.0001). They both positively correlated with congestion indexes (log hs-CRP, ePVS r = 0.2, HI r = 0.24, p < 0.0001 for both; log NLR, ePVS r = 0.20, HI r = 0.29, BUN/Cr 0.14, log brain natriuretic peptide (BNP) r = 0.16, p < 0.01 for all). After 90 days, the cumulative mortality rate was 26%. Inflammatory biomarkers (hs-CRP and NLR cutoffs were >60 pg/mL and >7.5, respectively) were predictors of death. By using all these parameters, we performed an index of inflammation (from 0 to 2) for each patient. Congestion and inflammation indexes were independent predictors of mortality (hazard ratios 1.4 and 2.3, respectively; C-index 0.72). Conclusion: Systemic inflammation seemed directly associated with congestion burden in patients with AHF. Both of them have different impacts on the prediction of adverse outcomes in these patients. Further studies are needed to address unmet needs.