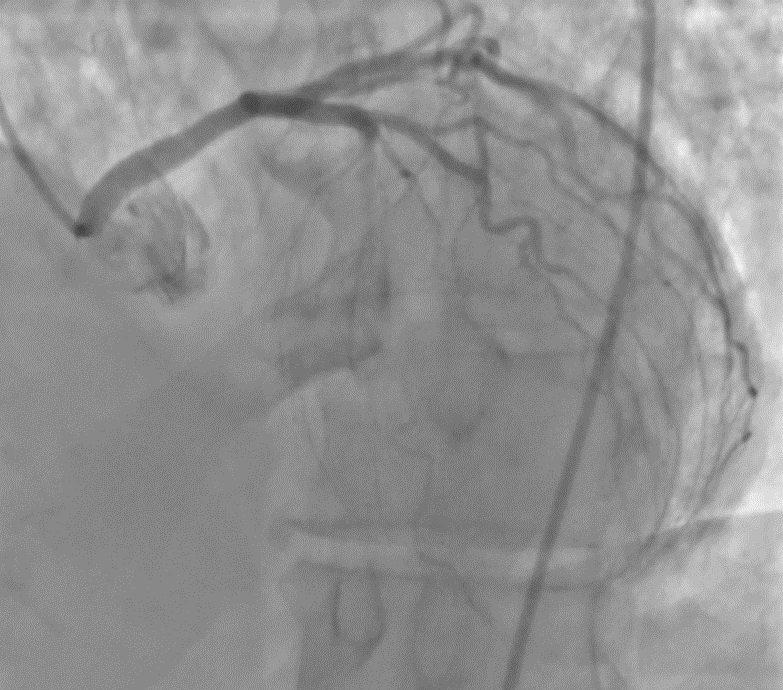
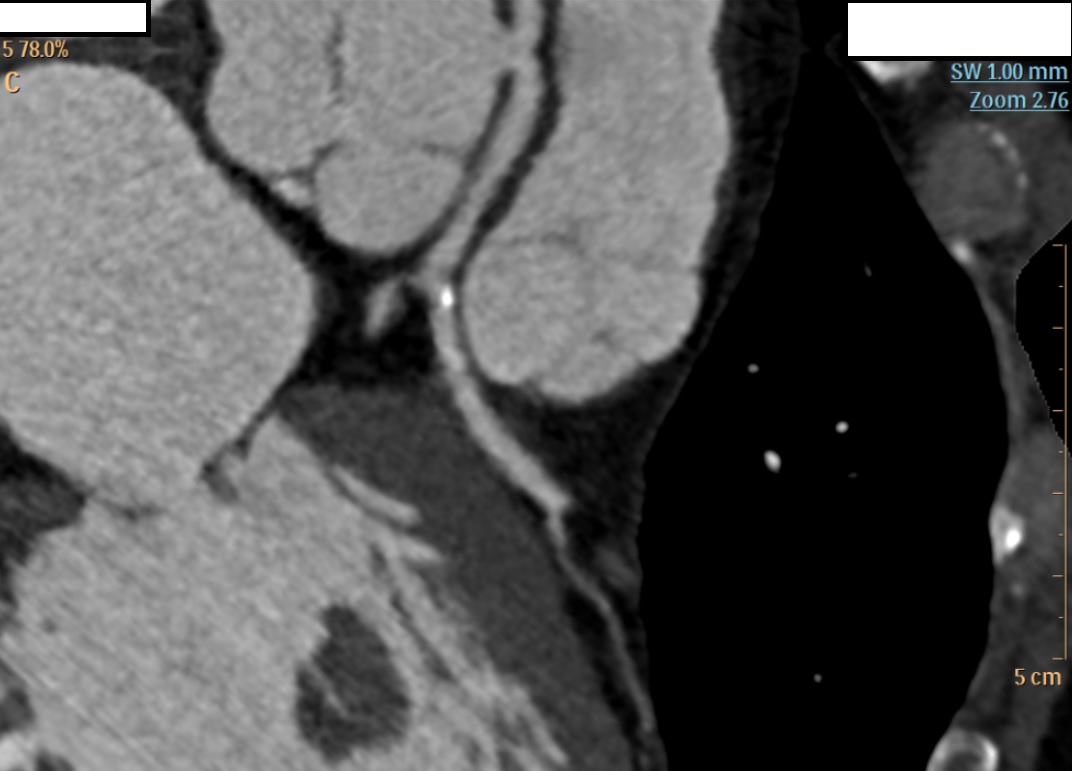
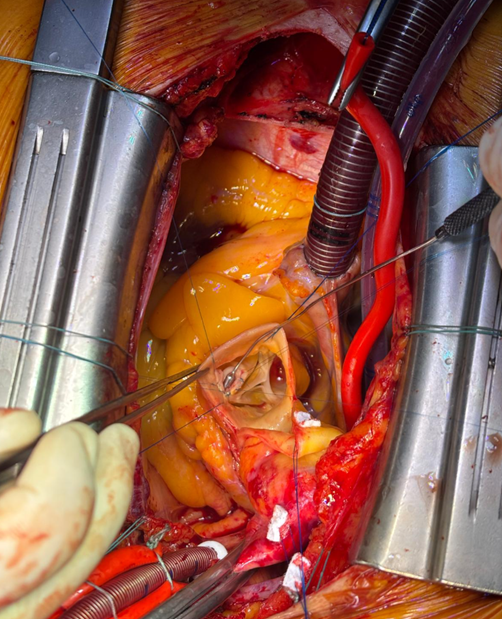
Background Congenital coronary artery anomalies have an estimated prevalence of approximately 1% in the general population. Some "malignant" variants, particularly the anomalous origin of the left coronary artery from the right sinus of Valsalva with an interarterial and/or intramural course, are associated with an increased risk of myocardial ischemia and sudden cardiac death. These anomalies are generally diagnosed at a young age, often during sports medicine screening. Case presentation A 63-year-old man was admitted to the cardiac intensive care unit after a witnessed out-of-hospital cardiac arrest occurring at rest, successfully treated in the pre-hospital setting for ventricular fibrillation with 2 defibrillation shocks and 1 mg of epinephrine. His medical history included treated arterial hypertension and known left bundle branch block (LBBB); occupation: butcher. On admission to the emergency department, electrocardiography showed sinus rhythm with LBBB, severe hypokalemia (K⁺ 2.6 mmol/L), and elevated troponin T (peak 205 ng/L). Transthoracic echocardiography (bad quality) revealed septal dyssynergy and mildly reduced left ventricular ejection fraction. Coronary angiography (CGF) showed no significant coronary stenoses and an ectopic origin of the left coronary artery from a non-coronary sinus, without clear definition of its course. Cardiac magnetic resonance imaging (MRI) was negative for fibrosis, necrosis, or myocarditis. During the diagnostic work-up, suspicious pelvic bone lesions were detected but subsequently ruled out as neoplastic by MRI and PET-CT. To complete the cardiological assessment, coronary computed tomography (CT) demonstrated origin of the left coronary artery from the right coronary sinus, with an acute take-off angle (<45°), a probable short intramural course, and an interarterial course between the aorta and pulmonary artery. Based on these findings, surgical correction with an unroofing procedure was indicated. Conclusions This case represents an atypical presentation of a "malignant" coronary anomaly given the age and mode of onset, occurring at rest in an adult patient. CGF and MRI may be insufficient in the anatomical characterization of coronary anomalies, while coronary CT remains the method of choice for defining the course and therapeutic strategy. Clinical suspicion remains a fundamental element in identifying causes of cardiac arrest that are only apparently idiopathic.