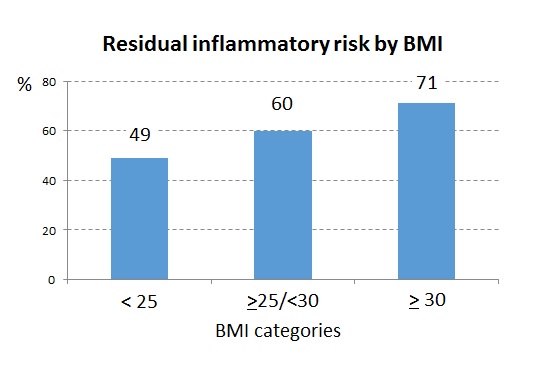
Background It is well known that residual inflammatory risk (RIR) is closely associated with prognosis in patients with acute coronary syndrome (ACS), independently of cholesterol levels achieved with high-intensity statin treatment. Subjects with a higher body mass index (BMI) often show a greater degree of systemic inflammation, highlighting BMI as a key factor in RIR. The aim of this retrospective analysis was to investigate the relationship between BMI and RIR at 1 month after ACS in patients treated with early invasive strategy and high-intensity statins from admission. Methods Patients with non ST elevation ACS, included in the PRATO-ACS Registry (ClinicalTrials.gov ID: NCT04087200), were stratified into three groups based on BMI: group 1 (underweight/normal weight, BMI <25), group 2 (overweight, BMI ≥25 and < 30) and group 3 (obese, BMI >30). One month after the acute event, RIR was defined as high-sensitivity C-reactive protein (hs-CRP) levels ≥ 2 mg/L. The association between BMI and hs-CRP at 1 month was evaluated with Cox proportional analysis. Results This study included 1094 subjects (68±12 years, 70.3% males), only 24.2% on statin therapy before admission. Percutaneous coronary intervention was performed in 68 % of cases. At 1 month the majority (59%) of patients had levels of hs-CRP above the risk cut-point. The percentage of patients with RIR increased progressively and significantly with increasing BMI (49% in group 1, 60% in group 2 and 71% in group 3, p<0.0001). Overweight and obesity were found to be independent predictors of RIR (adjusted odds ratios 1.5 and 2.3, respectively), together with age and diabetes, but not cholesterol levels. Conclusions In this population of ACS patients on high-intensity statin therapy BMI was independently associated with RIR at 1 month. Early intensification of secondary prevention measures, based not only on cholesterol values, could lead to a more targeted reduction in residual risk after ACS.