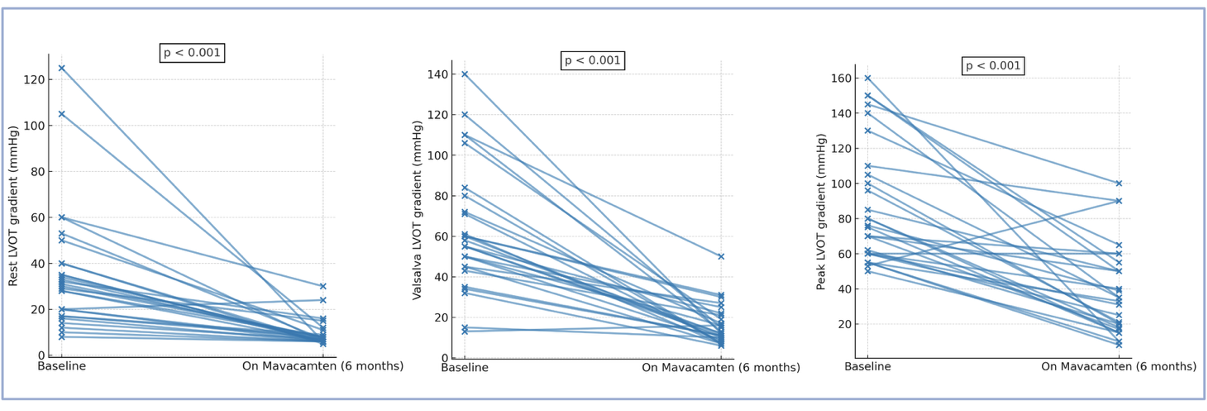
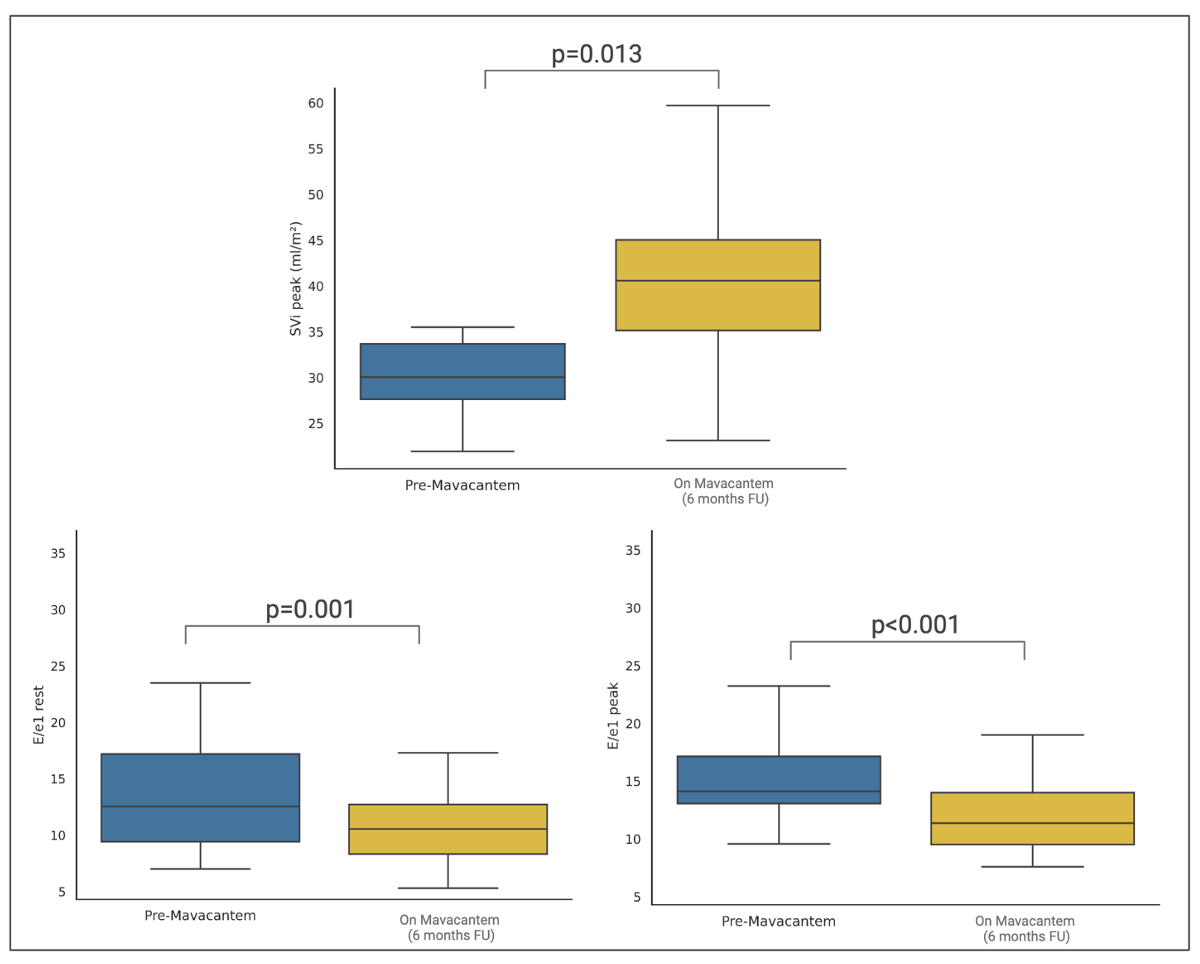
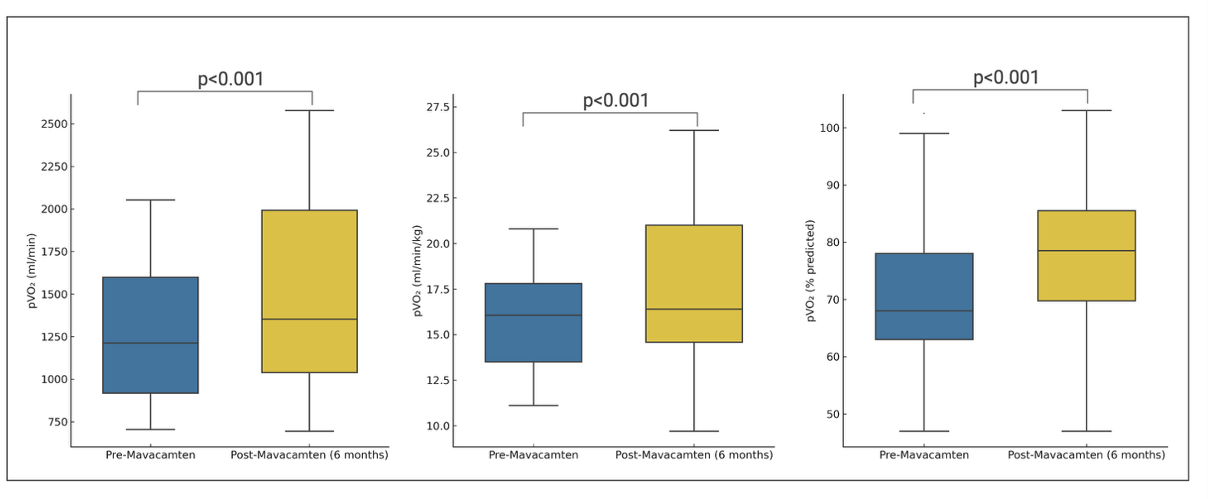
Background : Mavacamten, a selective cardiac myosin inhibitor, improves left ventricular outflow tract (LVOT) obstruction and symptoms in obstructive hypertrophic cardiomyopathy (HCM). However, real-world data integrating cardiopulmonary exercise testing (CPET) and echocardiography remain limited. Methods : In this prospective multicenter study, 28 patients with symptomatic obstructive HCM underwent transthoracic echocardiography and symptom-limited CPET at baseline and after 6 months of mavacamten therapy. The primary endpoint was the change in echocardiographic and CPET parameters. An exploratory secondary endpoint was the identification of baseline predictors of functional response, defined as a ≥5 percentage point increase in predicted peak oxygen consumption (%pred pVO₂). Results : After 6 months of treatment, resting LVOT gradient decreased from 30.5 [19.2–40.0] to 7.0 [6.0–8.2] mmHg (p = 0.001), and peak LVOT gradient from 75.5 [60.0–106.2] to 34.0 [17.8–51.2] mmHg (p = 0.001). Left atrial volume index and diastolic function indices significantly improved, with reductions in E/e′ at rest (12.6 [9.4–17.2] to 10.6 [8.3–12.7]; p=0.001) and at peak (14.1 [13.1–17.1] to 11.2 [9.3–13.8]; p = 0.001). Peak pVO₂ increased from 1213 [918–1598] to 1352 [1039–1992] ml/min (p= 0.001), pVO₂ ml/min/kg from 16.0 [13.5–17.8] to 16.4 [14.6–21.0] (p=0.004), and %pred pVO₂ from 68.0 [63.0–78.0] to 77.0 [69.5–86.0] (p=0.008). PETCO₂ at peak exercise increased (34.1 [31.2–35.6] to 35.4 [33.1–37.6]; p=0.002), and VE/VCO₂ slope decreased significantly (35.0 [32.7–37.0] to 31.6 [28.7–35.0]; p=0.007), indicating enhanced ventilatory efficiency. Overall, 46% of patients achieved a functional response (Δ%pred pVO₂ ≥+5). Lower baseline %pred pVO₂ (OR 0.58 [0.36–0.91]; p=0.021) and higher VE/VCO₂ slope (OR 1.56 [1.02–2.42]; p=0.041) independently predicted response, with fair model discrimination (AUC=0.73). Conclusions : Mavacamten significantly reduced LVOT gradients and improved diastolic, ventilatory, and functional parameters in obstructive HCM. Nearly half of patients experienced a clinically relevant improvement in exercise capacity, with baseline ventilatory inefficiency and lower aerobic performance identifying those most likely to benefit.